
The pinning was either lateral or crossed configuration with medial and lateral wires. Our inclusion criteria for the study involved any patient up to the age of 13 years who had a supracondylar humeral fracture and underwent closed reduction with percutaneous pinning within 24 h of the insult and with no neurological or vascular injury prior to the operation. A convenience sampling method was used to obtain our sample. Multiple parameters were reviewed, including gender, age, and surgical intervention, as well as scores for pain, ROM, function, and stability. This study reviewed a total of 101 cases of children with supracondylar humeral fractures that were presented to the emergency department of KAUH between 20. Before conducting this study, ethical approval was obtained from the Institutional Review Board (IRB) committee of KAUH. We conducted a single-blinded retrospective cohort study at the Department of Orthopedics of King Abdullah University Hospital (KAUH). 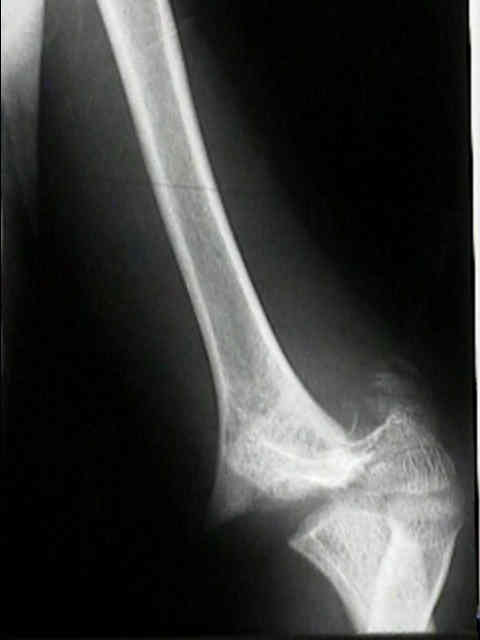
These may include measurement of Baumann angle (Figure 2), carrying angle, the development of complications, and the necessity to re-operate. Other measures with clinical-radiological value may be considered as well. In order to compare the two techniques, the well-validated Mayo elbow performance score (MEPS) was used as a standardized functional outcome measure. The null hypothesis was that there is no difference between the treatment groups. Therefore, this study aimed to study the difference in stability and functional outcomes between patients managed by lateral pinning and those managed by crossed pinning for displaced supracondylar fracture of the humerus. Conversely, lateral pinning may be less stable biomechanically but avoids ulnar nerve injury. Theoretically, crossed pinning is superior in providing biomechanical stability, yet this construct increases the risk of iatrogenic ulnar nerve injury due to the medial pin position. Controversy persists between the two perspectives regarding which is better in terms of fixation stability and risk of developing complications.įigure 1 Postoperative AP view radiographs. Elbow range of motion (ROM) and function are usually preserved, provided that adequate reduction is achieved through surgical intervention or casts application.ĬRPP has two techniques: Lateral pinning technique (Figure 1A) and cross pinning technique (Figure 1B). The most commonly reported postoperative complication is pin migration.ĭespite reported complications of neurovascular injuries, it has been well documented in the previous literature that pediatric supracondylar humerus fractures generally have good outcomes. Rarely, open reduction with percutaneous pinning is needed in open fractures and in cases of failed closed reduction. Pinning is performed retrogradely, using two pins for type 2 fractures and three pins for type 3 fractures. Operative management is almost always required in more severe types, including closed reduction and percutaneous pinning (CRPP). This involves long arm casting with less than 90 degrees of elbow flexion. In addition, the modified Gartland classification is frequently used, describing one more type, type 4 - complete multidirectional displacement of fragments with periosteal disruption.Īs for the management of these fractures, a trial of conservative management may be undertaken with type 1 fractures and minimally displaced type 2 fractures. It classifies them as type 1 - nondisplaced or minimally displaced, type 2 - displaced with intact posterior cortex, and type 3 - completely displaced without contact between fragments. The Gartland classification system is a popular system for the evaluation and treatment of these fractures. These fractures may be complete or incomplete with varying degrees of severity. They are most commonly seen in children 5-7 years of age with no gender predilection. These fractures are typical pediatric injuries, accounting for 60% of upper limb fractures and 13% of pediatric fractures. A supracondylar humeral fracture happens through the thin part of the distal humerus above the growth plate level.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
